As our Supporting Providers Positively work in Norfolk draws to a close next week, I’ve been reflecting on what we’ve learned so far and what has genuinely made a difference.
We’ll be completing a second impact report shortly, capturing the full scope of the project. But before we do that, it felt important to share some of the early findings from our first evaluation.
Because too often in social care, we talk about frameworks, standards, and expectations… without really understanding what improves day-to-day practice.
Read the full Impact Report here:
Moving beyond compliance
At Supporting Positively, our work is grounded in a simple principle:
Good care doesn’t come from preparing for inspection it comes from building environments where good practice is the default.
Through our Supporting Providers Positively model, we’ve focused on helping services develop capable environments. This means places where:
- Staff feel confident, skilled, and supported
- Practice is consistent and predictable
- People experience meaningful, person-centred support
- Quality of life is the central focus
This isn’t about adding more processes.
It’s about strengthening what happens every day, in real interactions.
What we saw in Norfolk
1. Confidence and energy within staff teams
One of the earliest and most consistent impacts was on staff confidence and morale.

This matters because confident staff are more likely to:
- Respond proactively
- Use PBS principles consistently
- Support people in more meaningful ways
And this shift didn’t come from training alone; it came from modelling, reflection, and doing the work together.
2. From variation to consistency
Across services, one of the biggest shifts was in consistency of support.
Providers began developing:
- Shared approaches
- Clearer systems
- More predictable support environments
This is reflected in baseline findings, where:
- 66% of providers identified systems as an area for improvement
- 35% identified a need to strengthen staff skills to embed PBS
And through the work, we saw those gaps begin to close
3. Measurable improvements in practice
Where providers completed the full model, we saw statistically significant improvements (p < 0.01) across targeted areas of Capable Environments
Some examples included:
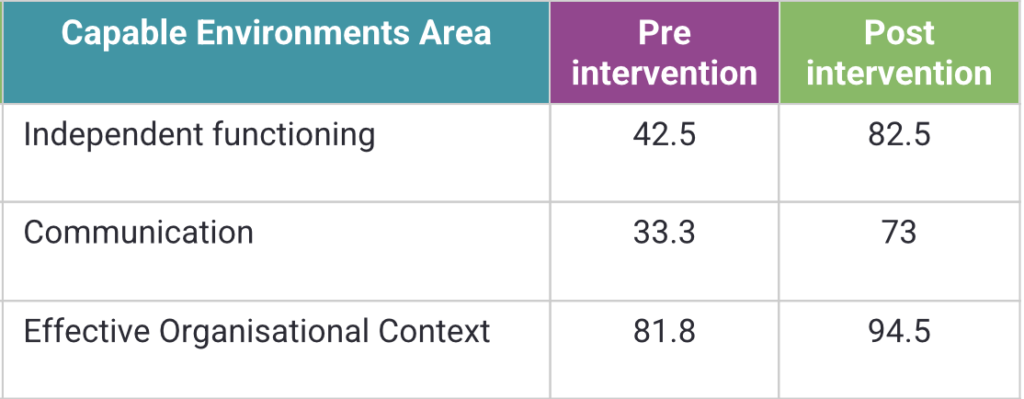
This is important.
Because it shows that when you focus on environment, systems, and staff capability, improvement is not just possible, it’s measurable.
4. Reducing restrictive practices through ownership
Rather than imposing change, the approach focused on engagement and ownership.

This is where real change happens.
Not through policy alone, but through:
- Clear focus and support
- Small, meaningful changes
- Staff-led action
5. Real outcomes that matter
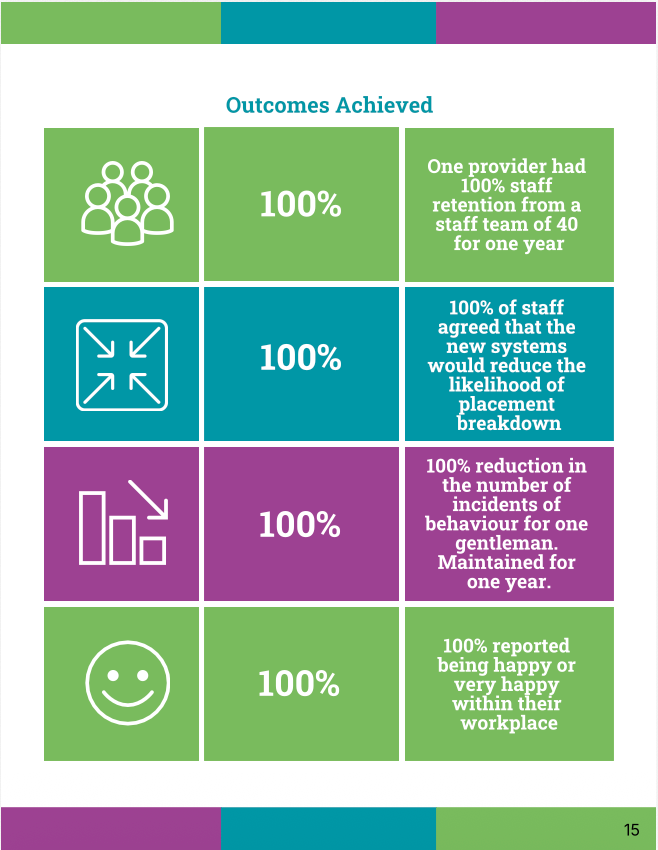
Beyond systems and scores, the outcomes were tangible:
- 100% reduction in incidents for one individual (maintained for a year)
- 100% staff retention in one service (team of 40)
- 100% of staff agreed new systems reduced likelihood of placement breakdown
And perhaps most importantly:
- 100% of staff reported being happy or very happy in their workplace
These are the outcomes that matter, not just compliance, but stability, wellbeing, and quality of life.
6. A shift in culture
Across the work, there was a noticeable shift in how services thought about improvement.

And more broadly, services began moving from:
“What do we need to do for CQC?” to “What does good support actually look like here and how do we sustain it?”
That shift is what creates lasting change.
Why this matters now
With increasing focus from regulators on defining “what good looks like”, there’s a real opportunity for the sector.
But there’s also a risk.
If we focus only on frameworks and guidance, without supporting services to embed them, we will continue to see the same gap:
Knowing what good looks like vs Being able to deliver it consistently
Our experience in Norfolk reinforces this:
Improvement happens when we invest in environments, not just expectations.
What comes next
This project is now drawing to a close, and we’ll shortly be completing a second impact report to reflect the full journey and longer-term outcomes.
I’m really looking forward to sharing that in the coming weeks.
Final reflection
There’s no shortage of guidance in social care.
What we need is more focus on:
- Practice
- Culture
- Environment
- And the lived experience of the people we support
Because that’s where real quality lives.

